CHAPTER VI
Heart and Lung Transplantation in the United States, 1997-2006
OVERVIEW
The number of candidates awaiting heart transplantation declined by 45%, from 2,414 patients in 1997 to 1,327 patients in 2006. Death rates among candidates declined over the same period. Deaths in the first year after heart transplantation steadily decreased over the decade.
At the end of 2006, 2,885 candidates were awaiting a lung transplant, up 10% from 1997. The median time-to-transplant for listed patients decreased by 87%, from 1,053 days in 1997 to 132 days in 2006.
Selection for listing and transplantation has shifted toward more urgent patients since 2005, when a new lung allocation system began. The new system is based on survival benefit and urgency rather than waiting time alone.
Only 31 heart-lung transplants were performed in 2006, down from 62 in 1997.
This chapter reviews recent trends in heart and lung transplantation in the United States. The data reported here are drawn from the 2007 OPTN/SRTR Annual Report, and cover all aspects of thoracic organ transplantation in the last decade. Two recent changes in the allocation systems for these two organs — the Lung Allocation Score system, introduced in May 2005, and the increased geographic sharing of hearts, introduced in July 2006 — seem to be having noticeable effects on transplantation trends. Both systems were introduced in order to save lives. The data available for evaluating the beneficial effects of these allocation changes are not yet quite mature, but interesting trends are becoming apparent, as described throughout this paper. Critics have challenged some of the early data interpretation of these changes, as preliminary analyses (like the statistical models behind the changes themselves) were based on one-year risk of patient death, rather than longer-term risk. Five-year survival rates were not used to develop these allocation systems, but they will be valuable when they become available. Revisions in both allocation schemes are ongoing, as factors are identified that may enhance the systems’ ability to make the best use of this scarce resource.
[TOC]Heart Waiting List Characteristics
[TOC]The characteristics of heart transplant candidates are derived from potential transplant recipients actively awaiting heart transplantation at the end of each calendar year from 1997 to 2006 [Table 11.1a]. Overall, the total number of active candidates declined by 45% over the decade, dropping from 2,414 patients in 1997 to 1,327 patients in 2006 [Table 11.1a].
The percentage of patients actively awaiting heart transplantation with blood type O increased by approximately 9% over the last 10 years. Other characteristics of heart transplant candidates, including country of residence, history of previous transplant with any organ, or history of previous heart or lung transplant, remained relatively unchanged (<2% change) from 1997 to 2006.
Patients awaiting heart transplantation are assigned a level of urgency based on medical condition and include, from most to least urgent: Status 1A, Status 1B, and Status 2. A Status 1A candidate has either mechanical circulatory support for acute hemodynamic decompensation, mechanical circulatory support with objective medical evidence of device-related complications, continuous mechanical ventilation or intra-aortic balloon pump, or continuous infusion of intravenous inotropes along with continuous monitoring of left ventricular filling pressures. Additionally, a patient may be listed as Status 1A in the absence of these conditions if the transplant physician submits an application for Status 1A to the Regional Review Board and the application is approved. The decision of the Regional Review Board is also reviewed by the OPTN Thoracic Organ Transplantation Committee if the assessment of the Regional Review Board is appealed by the transplant center. Status 1B covers candidates with a left or right ventricular assist device implanted and candidates receiving a continuous infusion of intravenous inotropes without the specific requirement of continuous monitoring of left ventricular filling pressures. A candidate not meeting the conditions for Status 1A or Status 1B may be listed as Status 2. Most candidates for heart transplantation are listed as Status 2; this has consistently been the case since 1997 [Table 11.1a]. Since 1999, there has been a 51% decrease in number of patients listed as Status 2, an 18% decrease in number of patients listed as Status 1B, and a 14% decrease in patients listed as Status 1A. These changes have resulted in a relative increase in the proportion of candidates listed at Status 1A or 1B. The proportion of patients listed at each Status has remained relatively constant since 2004 (Figure VI-1).
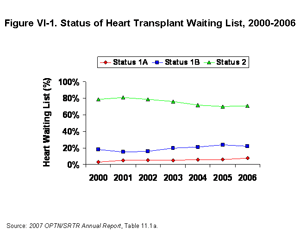 | Click for larger image Click to view slides for entire chapter |
Overall, the distribution of time spent on the heart transplant waiting list did not change appreciably from 1997 to 2006, although there was a small increase (approximately 6%) in the percentage of patients awaiting heart transplantation for two or more years [Table 11.1a]. This increase was seen primarily in the type O blood group, while there was a slight decrease in type A and types B and AB were virtually unchanged. Of the 78 patients awaiting heart transplantation and listed as Status 1A as of January 1, 2006, 27%, 17%, and 14% of patients remained listed as Status 1A at the end of 30, 60, and 90 days, respectively [Table 11.2b]. The percentages of patients initially listed at Status 1A who received a heart transplant were 37%, 54%, and 58% at 30, 60, and 90 days, respectively [Table 11.2b]. For the 324 patients awaiting transplantation and listed as Status 1B as of January 1, 2006, 75%, 58%, and 46% remained listed as Status 1B at 30, 60, and 90 days, respectively, while 12%, 24%, and 34% of patients received transplants at 30, 60, and 90 days, respectively [Table 11.2b]. For patients listed as Status 2, only 6%, 8%, and 11% received a heart transplant by 30, 60, and 90 days, respectively [Table 11.2b].
Deaths on the Heart Waiting List
[TOC]The overall death rates among patients awaiting heart transplantation have declined over the last 10 years, from 227 per 1,000 patient-years at risk in 1997 to 152 per 1,000 patient-years at risk in 2006 (Figure VI-2) [Table 11.3]. This trend was clearly evident regardless of ethnicity, sex, blood type (except blood group AB), age (except for patients <1 year old), and diagnosis (except for retransplant/graft failure/unknown). Death rates on the heart waiting list decreased sharply among Status 1A candidates, from 2,087 deaths per 1,000 patient-years at risk in 2000 to 1,457 deaths per 1,000 patient-years at risk in 2006 (Figure VI-3). Death rates among Status 1B and Status 2 patients declined as well, though less sharply and with more year-to-year variability (Figure VI-3). The increasing prevalence of ventricular assist device (VAD) placement may have contributed to the declining death rates, particularly among Status 1A patients.
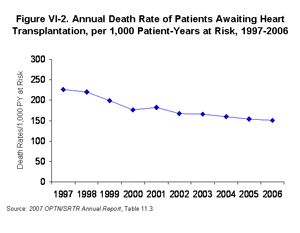 | Click for larger image Click to view slides for entire chapter |
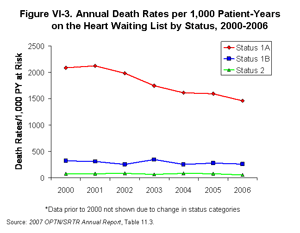 | Click for larger image Click to view slides for entire chapter |
Heart Transplant Recipient Characteristics
[TOC]The overall number of heart transplants performed has varied by 14% over the past decade, from a high of 2,348 in 1998 to a low of 2,015 in 2004 [Table 11.4]. After reaching a 10-year low in 2004, the number of transplants increased slightly in each of the past two years. There was also a 14% decrease in the rate of heart transplants per million U.S. residents over the last 10 years, though this trend appears to have leveled off over the last few years (Figure VI-4) [Table 11.5]. Among patients transplanted, there has been an 18% decrease in the 50-64 age group, a 19% reduction in the number of white recipients, and a 24% reduction in the number of patients transplanted with a diagnosis of coronary artery disease [Table 11.4]. As with changes in waiting list characteristics, these changes have resulted in greater percentages of patients receiving transplants among younger age groups, non-whites, and candidates with a diagnosis other than coronary artery disease. Other important trends have included a 51% reduction in the number of patients hospitalized in an intensive care unit before heart transplantation and a reciprocal increase in the number of patients hospitalized outside an intensive care unit or not hospitalized at all before heart transplantation [Table 11.4]. There has also been a 17% reduction in the number of patients on life support (extracorporeal membrane oxygenation, intra-aortic balloon pump, prostaglandins, intravenous inotropes, inhaled nitric oxide, ventilator) at the time of heart transplantation over the past decade. There have been no significant changes in the characteristics of heart transplant recipients with respect to sex (approximately 75% of heart recipients are male), recipient blood type, previous transplant with any organ, previous heart or heart-lung transplant, and recipient residency [Table 11.4].
 | Click for larger image Click to view slides for entire chapter |
The distribution of patients among the different status groups on the waiting list at the time of heart transplantation changed little between the inception of the new classification system in 1999 and 2005. At that time patients at Status 1A, 1B, and 2 at the time of transplantation comprised approximately 40%, 35%, and 25%, of the entire cohort [Table 11.4]. However, in 2006 the proportion of Status 2 patients dropped to 20%, while Status 1A and 1B patients increased to 42% and 38% respectively (Figure VI-5). This change is likely attributable to the wider geographic sharing of donor hearts for candidates at Status 1A or 1B as a result of the change in donor heart allocation process approved by the OPTN Board of Directors in November 2005 and implemented in July 2006 (1). The policy was expected to lead to a decrease in Status 2 transplants in favor of candidates listed at a more urgent status. Despite an increase in the geographic sharing of donor hearts for candidates at Status 1A or 1B, there was only a 1% increase in the number of donor organs with cold ischemic time between 270-360 minutes from 2005 to 2006 compared to earlier years. Other cold ischemic time categories had even less of an increase or no increase at all.
 | Click for larger image Click to view slides for entire chapter |
Immunosuppression Therapy for Heart Transplantation
[TOC]The immunosuppression regimen for heart transplant recipients has continued to evolve over the past decade [Table 11.6a]. Induction therapy in the form of Atgam® (equine antithymocyte globulin) or OKT3® (muromonab-CD3) was used for 30% of patients in 1997. While use of induction therapy has gradually increased, reaching 57% in 2006, both Atgam and OKT3 have been largely replaced by the use of Thymoglobulin® (rabbit anti-lymphocyte globulin) or monoclonal antibody therapy directed against the IL-2 receptor — namely, Zenapax® (daclizumab) or Simulect® (basiliximab) [Table 11.6a]. Over the past decade, the overwhelming majority (approximately 80%) of transplant recipients were discharged on triple drug therapy consisting of a calcineurin antagonist, mycophenolate mofetil (MMF) / myocophenolic acid (MPA) or other antimetabolite, and steroid therapy [Table 11.6d]. The two most common regimens in 1997 (75% of transplant recipients) were cyclosporine (CyA) with either mycophenolate mofetil / myocophenolic acid or another antimetabolite and steroids. These combinations have evolved to predominantly tacrolimus (Tac), mycophenolate mofetil / myocophenolic acid, and steroids (49% of transplant recipients) — and, to a lesser extent (29% of transplant recipients), cyclosporine, mycophenolate mofetil / myocophenolic acid, and steroids. At one year following transplantation, triple drug therapy with a calcineurin antagonist (principally tacrolimus), mycophenolate mofetil / myocophenolic acid, and steroid therapy remains the predominant treatment regimen [Table 11.6f]. However, since 1997 there has been a small (approximately 15% of patients) but important trend towards steroid-free drug regimens by one year following transplantation. Heart transplant recipients discharged on tacrolimus and mycophenolate mofetil / myocophenolic acid, with or without steroid therapy, have the greatest likelihood of remaining on this drug regimen, compared to all other drug combinations at three years following transplantation [Table 11.6h]. A notable trend is the declining number of recipients who needed treatment for rejection episodes during the first year following transplantation (25% in 2005 compared to 36% in 1996) [Table 11.6i]. The overwhelming majority of patients were treated with steroid therapy while approximately 18% were treated with some form of antibody therapy. The decline probably reflects the improved efficacy of the newer immunosuppression medications, but also may result from incremental improvements in the overall care of donors and recipients. The incidence of infection and malignancy require further analysis to identify meaningful trends.
[TOC]Deaths in the first year after heart transplantation have steadily decreased from 171 deaths per 1,000 patient-years at risk in 1997 to 132 deaths per 1,000 patient-years at risk in 2003 (Figure VI-6) [Table 11.7]. There has been a slight increase the incidence of death during the last two years, to 142 deaths per 1,000 patient-years at risk. Adjusted to the characteristics of the 1996 heart transplant population (age, sex, race, and diagnosis), patient survival at three months and one year improved from 89.7+0.6% and 85.2+0.7%, respectively, in 1996, to 92.1+0.6% and 87.8+0.7%, respectively, in 2005 [Table 11.13]. Long-term survival at three and five years increased from 77.3+0.9% and 70.8+1.0%, respectively, in 1996, to 79.2+0.9% and 73.7+1.0% in 2001, the most recent year with adequate Post Transplant follow-up (Figure VI-7) [Table 11.13]. Adjusted graft survival was nearly identical to adjusted patient survival. The prevalence of people living with a functioning heart allograft at year-end increased every year from 13,829 in 1997 to 18,018 in 2005 [Table 11.16].
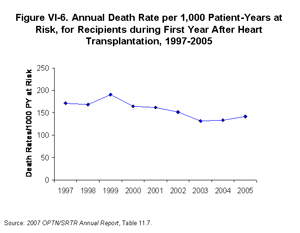 | Click for larger image Click to view slides for entire chapter |
 | Click for larger image Click to view slides for entire chapter |
There has been variability in how Post Transplant death rates have declined since 1997. The downward trajectory of one-year death rates was more marked among African Americans and Hispanics and has brought them more into line with the one-year death rates of whites [Table 11.7]. African Americans experienced somewhat worse survival starting at three years after transplantation relative to other ethnicity groups. Downward trends in death rates have had more year-to-year variability among the smaller number of Asian transplant recipients (Figure VI-8). Death rates for females and males were similar in 2005, though females generally have had a higher death rate over the last 10 years [Table 11.12].
 | Click for larger image Click to view slides for entire chapter |
Congenital heart disease patients have seen worse Post Transplant survival than have patients with coronary artery disease, valvular heart disease, and cardiomyopathy. In general, there has been a decline in death rates among all status groups since 1999; however, in 2005 there was an increase over 2004 rates in both Status 1A and Status 2 groups. Status 1B experienced a sharp decrease in 2005 compared to 2004 (Figure VI-9). In 2005, annual death rates per 1,000 patient-years at risk during the first year after transplantation remained highest for those 1-5 years old or those 65 years or older, with death rates of 245 and 176, respectively [Table 11.7]. A one-year death rate of 63 per 1,000 patient-years at risk set a new 10-year low for patients aged 11-17 in 2004, but this rate returned to 172 in 2005, reflecting the year-to-year variability witnessed in this group over the last decade. By diagnosis from highest to lowest, the death rates in 2005 were 323 for congenital heart disease, 143 for coronary artery disease, 112 for cardiomyopathy, and 105 for valvular heart disease.
 | Click for larger image Click to view slides for entire chapter |
Heart Allocation Policy Changes
[TOC]In July 2006, the OPTN Thoracic Organ Transplantation Committee implemented an allocation policy change moving Zone A 1A and 1B patients ahead of local Status 2 patients (1). It is predicted that the policy change will result in fewer deaths on the waiting list and overall. However, very little follow-up has yet been accrued, even for those patients transplanted earliest during the era affected by the policy change. While some impact from the policy change may be reflected in the trends described above, it is expected that a more comprehensive review of the new policy’s effect can be made in future reports, after sufficient numbers of patients have received transplants under the new system and adequate follow-up has been accrued.
[TOC]The lung transplantation section of this chapter is organized differently than the heart section because policy changes following the institution of the Lung Allocation Score (LAS) system are most logically reviewed in terms of deaths on the waiting list and following transplantation. Rather than a discussion of waiting list characteristics and outcomes followed by a discussion of transplant recipient characteristics and outcomes, the discussion of waiting list and transplant characteristics and outcomes is combined.
[TOC]At the end of 2006, 2,885 candidates were registered on the lung waiting list and awaiting a transplant. This figure represents a 9% drop from the 2005 count of 3,156, following an 18% drop from 3,866 in 2004 [Table 1.3]. The change between 2005 and 2006 is almost entirely due to a decrease in the number of inactive registrants, as the number of registrants active on the lung waiting list remained steady between 2005 and 2006 at approximately 1,000 patients, down from 2,163 patients in 2004 (Figure VI-10) [Table 12.1a]. Many of the sections below describe year-over-year trends and changes from 2005 to 2006; it is also important to note that many of these trends (for instance, the waiting list numbers described above) were relatively stable for the previous decade, and underwent a pronounced change upon the introduction of the LAS system in May 2005.
 | Click for larger image Click to view slides for entire chapter |
The percentage of actively listed patients waiting less than 6 months for a transplant was 42% at the end of 2006, as opposed to only 32% of patients at the end of 2004, although the number of patients waiting less than a year was roughly 55% in each case [Table 12.1a]. The numbers of patients waiting more than one year for a transplant dropped substantially from 967 in 2004 to 452 in 2006 (a 53% decrease).
The median time-to-transplant for listed patients decreased by 87% over the decade, dropping from 1,053 days in 1997 to 132 days in 2006 (Figure VI-11) [Table 12.2]. Most of this decrease was seen between 2004 and 2006. In 2006, 10% of wait-listed patients received an organ within 9 days of being listed and 25% of listed patients received an organ within 31 days of listing.
 | Click for larger image Click to view slides for entire chapter |
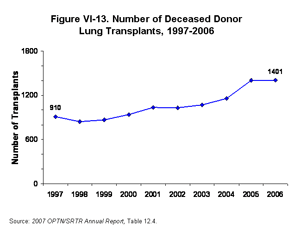
The waiting list death rate dropped by 48% between 1997 and 2006, from 185 to 97 deaths per 1,000 patient-years at risk (Figure VI-12) [Table 12.3]. Forty-three percent of this decrease occurred between 2004 and 2006 (135 to 97 deaths per 1,000 patient-years at risk). The smaller number of candidates, shorter accrued waiting times, and markedly reduced death rates on the waiting list between 2004 and 2006 are likely to be attributable in large part to the recent change in the lung allocation policy. Selection for listing and transplantation has shifted toward more urgent patients since implementation in May 2005 of the LAS system, which is based on survival benefit and urgency rather than waiting time (2). In addition, the Organ Donation Breakthrough Collaborative has helped organize efforts toward increasing the pool of available organs for transplantation (3). The number of deceased donor lung transplants increased by 54% over the past decade, from 910 in 1997 to 1,401 in 2006. Roughly half of this increase was seen between 2004 and 2005; the number changed little between 2005 and 2006 (Figure VI-13). The use of DCD lung transplants remains uncommon but increased from 3 in 2003 to 11 in 2006 [SRTR analysis].
 | Click for larger image Click to view slides for entire chapter |
 | Click for larger image Click to view slides for entire chapter |
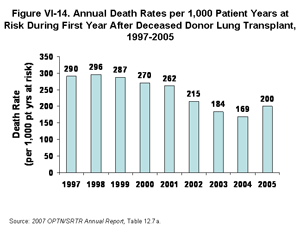
The reduced death rates on the waiting list since 2004 were offset by increased death rates observed between 2004 and 2005 in the first year after transplant with a deceased donor lung [Table 12.7a], likely a consequence of selecting more urgent patients for transplantation. The average death rate in the first year after transplantation decreased steadily from 290 per 1,000 patient-years at risk in 1997 to 169 deaths per 1,000 patient-years at risk in 2004, a 10-year low. The death rate in the first year following transplantation rose back up to 200 per 1,000 patient-years at risk (Figure VI-14) for transplants occurring during 2005. However, despite the increase in the one-year Post Transplant death rate for 2005, the total number of deaths on the waiting list and after transplant decreased by 2% in 2005 from 1,172 deaths in 2004 to 1,147 in 2005 [Table 12.3 and SRTR analysis]. (Here, and in subanalyses below, the total number of deaths includes all deaths after transplant during the year, regardless of when the transplant occurred.) Taken in combination, the net gain was 5.5 deaths prevented per 1,000 patient-years at risk. It remains to be seen whether this pattern will continue and how long-term death rates may alter the picture of net gain. The increases in Post Transplant death rates between 2004 and 2005 can likely attributed to sicker patients being selected for transplant during these years. It should also be noted that the total number of deaths presented here do not account for patients who may have been removed from the list due to being too ill to receive a transplant and subsequently died. Since May 2005 more acutely ill patients have been listed for transplantation, and it is probable that some are indeed removed from the waiting list and die shortly thereafter. Consequently, a composite risk of death for all patients may not be completely captured by the data presented here.
 | Click for larger image Click to view slides for entire chapter |
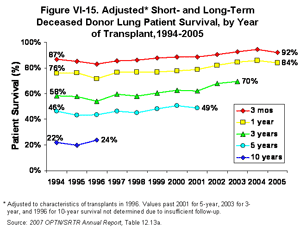
Once adjusted for age, race, sex, and diagnostic characteristics of the 1996 transplant cohort, Post Transplant patient survival rates were comparable to those seen in previous years, 92% at three months and 84% at one year [Table 12.13a]. (It is important to note that disease severity was not adjusted for in these comparisons, as much more information is available now than was available in 1996.) Three-year survival rates for these patients will not be available for another two years. (Figure VI-15).
 | Click for larger image Click to view slides for entire chapter |
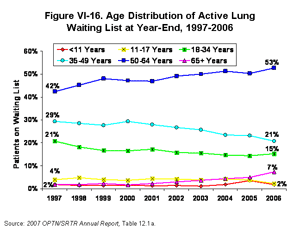
The age distribution of active patients on the lung waiting list has changed over the past decade (Figure VI-16) [Table 12.1a]. The percentage of patients 50 and older increased from 44% in 1997 to 60% in 2006. The percentage of patients 18-49 decreased from 50% in 1997 to 36% in 2006, and the percentage of patients 11-17 decreased from 4% to 2% [Table 12.1a]. With the exception of the shift in the percentage of adolescents on the waiting list, which occurred almost entirely between 2004 and 2006, most of these distributional shifts were already occurring during the eight years before implementation of the new lung allocation policy. These trends in changing age distribution simply continued between 2004 and 2006.
 | Click for larger image Click to view slides for entire chapter |
Although there were only relatively small shifts in the age distribution of patients on the waiting list between 2004 and 2005, the absolute numbers of patients decreased by at least 50% in all but the youngest and oldest age groups. The number of patients age 65 and above and those aged 6-10 also decreased but by only 21% and 36% respectively. The numbers of patients on the waiting list remained fairly steady between 2005 and 2006 for patients aged 18 to 64.
Except for very young children — for whom rates are unstable because of the small numbers of patients and deaths — patients aged 65 years and older had the highest waiting list death rates in 2006, followed by 11-17 year olds and 50-64 year olds. Candidates aged 18-34 and 35-49 had the lowest death rates [Table 12.3].
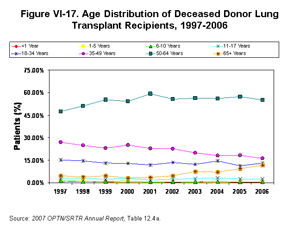
The number of transplants among patients less than 18 years old was fairly constant from 2004 to 2006 [Table 12.4a]. Transplants among 18-49 year olds increased approximately 9%-10% since 2004. Transplants among patients over age 50 have more than kept pace with the increases in the number of wait-listed patients in this age group, with a 28% increase in transplants since 2004 and a 97% increase since 1997. In 2006, 936 transplants occurred in patients older than 50 years. The percentage of patients aged 50-64 receiving transplants has not changed substantially since 2004, with 55% of deceased donor lungs going to these patients in 2006, up slightly from 48% in 1997 (Figure VI-17). However, between 1997 and 2006, the number of lung transplants in patients over age 65 nearly quadrupled (42, 81, and 164 transplants in 1997, 2004, and 2006, respectively) [Table 12.4a]. In 2006, patients 65 years or older represented 12% of all lung transplant recipients (Figure VI-17).
 | Click for larger image Click to view slides for entire chapter |
Since the implementation of the LAS system, first-year Post Transplant death rates have increased for all age groups. Since 1997, the highest first-year Post Transplant death rate has generally been seen for recipients 65 years or older, with 251 deaths per 1,000 patient-years at risk for patients who received a transplant during 2005 [Table 12.7a]. First year Post Transplant death rates for patients aged 18-34, 35-49 and 50-64 decreased until 2004 [Table 12.7a]. Again, there was an increase in the death rates for each of these age groups in 2005, likely related to more urgent patients being considered for transplantation.
For all age groups other than 11-17 year olds, the total numbers of deaths on the waiting list and following transplantation changed little from 2004 to 2005. Between 2004 and 2005, total deaths among patients aged 11-17 dropped from 38 to 29, a 24% decrease. The other age groups experienced smaller changes in total deaths. Total deaths among patients aged less than 11 remained constant, among patients aged 18-34 dropped by 5%, among patients aged 35-49 rose by 5%, among patients aged 50-64 dropped by 4%, and among patients 65 and older rose by 6% [Table 12.3 and SRTR analysis].
Lung: Breakdown by Diagnosis Groups
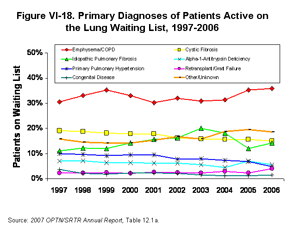
[TOC]The diagnosis distribution of wait-listed patients changed noticeably between 2004 and 2006. The most pronounced shifts were seen in the percentage of patients with idiopathic pulmonary fibrosis (IPF), which decreased from 18% to 14% of listed patients, and the percentage of patients with chronic obstructive pulmonary disease (COPD), which increased from 31% to 36% of listed patients (Figure VI-18) [Table 12.1a]. This change reflects, in part, a relative increase in the number of IPF patients transplanted due to higher LAS than that of COPD patients [Table 12.4a].
 | Click for larger image Click to view slides for entire chapter |
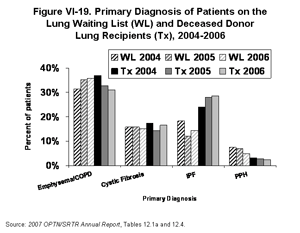
Despite this shift, emphysema and COPD remain the most common diagnoses leading to transplantation (Figure VI-19). At the end of 2006, 435 emphysema/COPD patients received transplants (31% of all transplants), while 371 continued to wait (36% of candidates); corresponding percentages for other major diagnoses include the following: IPF (29% of transplants, 14% of candidates), cystic fibrosis (17% of transplants, 15% of candidates), and primary pulmonary hypertension (2% of transplants, 5% of candidates) [Tables 12.4a and 12.1a]. Waiting time has dropped dramatically for all diagnosis groups since 2004. Although most of the change occurred between 2004 and 2005, there were further decreases in waiting time in 2006, particularly for primary pulmonary hypertension (PPH) patients whose waiting times had been 2 to 7 times longer than other groups in 2004 and 2005. In 2006, PPH patients continued to have the longest waiting times among these diagnosis groups, but the differences in waiting time were much smaller than in 2005 [SRTR analysis].
 | Click for larger image Click to view slides for entire chapter |
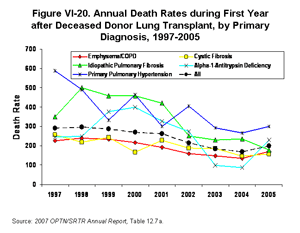
For all diagnosis groups other than IPF, there were declining first-year Post Transplant death rates until 2004 followed by increased rates in 2005 (Figure VI-20) [Table 12.7a]; IPF death rates continued to fall, reaching a 10-year low in 2005, when the LAS was implemented. Throughout the same decade emphysema/COPD and cystic fibrosis (CF) recipients had similar death rates, trending lower than patients with other underlying diagnoses. PPH patients had the highest one-year Post Transplant death rates in 2005, roughly 70%-90% higher than the death rates of the other most common diagnoses (Figure VI-20) [Table 12.7a]. Fortunately, five-year adjusted survival is more comparable for these diagnosis groups (PPH: 51%; CF: 52%; IPF: 51%; emphysema/COPD: 54%) [Table 12.12].
 | Click for larger image Click to view slides for entire chapter |
Between 2004 and 2005, the death rate on the waiting list decreased for all of the most common diagnosis groups while the death rate in the first year after transplant increased for all but IPF patients (Figure VI-21). The total number of deaths on the waiting list and after transplant (including all deaths after transplant during the year, regardless of when the transplant occurred) however decreased for all of the diagnosis groups. In 2005, total deaths among PPH patients dropped from 57 to 53 (7%), among CF patients dropped from 196 to 166 (15%), among IPF patients dropped from 280 to 258 (8%), and among emphysema/COPD patients dropped from 389 to 370 (5%) [Table 12.3 and SRTR analysis].
 | Click for larger image Click to view slides for entire chapter |
The percentage of patients waiting for a retransplant increased from 3% in 2004 to 4% in 2006, although the actual number of such candidates decreased from 67 in 2004 to 44 in 2006 [Table 12.1a]. In 2005-2006, 128 patients with a previous lung or heart-lung transplant were retransplanted with a deceased donor lung, more retransplants than were performed in the previous four years combined [Table 12.4a]. In 2005, 305 deaths per 1,000 patient years were observed among patients with any previous transplant, a 57% higher death rate than seen for recipients without previous transplants [Table 12.7a]. These trends of increasing Post Transplant mortality for patients rejoining the lung waiting list must be monitored closely. Further analysis of the risk-benefit profile for retransplantation and appropriate policy changes in lung allocation scoring should be considered as results emerge.
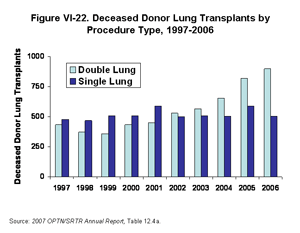
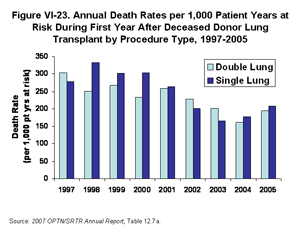
The number of bilateral lung transplants has more than doubled over the decade, rising from 432 (48% of deceased donor lung transplants) in 1997 to 897 (64% of transplants) in 2006 (Figure VI-22) [Table 12.4a]. In 2005, first-year Post Transplant death rates were 7% lower for double-lung recipients than for single-lung recipients, although this comparison does not adjust for multivariate factors such as diagnosis and age (Figure VI-23) [Table 12.7a]. Because the survival advantage conferred by a double lung transplant is still unclear, further analysis is needed, including the impact on organ utilization of more double lung transplants being performed. Appropriate use of marginal donor lungs typically mandates double lung transplantation. Consequently, the liberal performance of double lung transplantation may not hinder aggressive and appropriate use of available donor lungs.
 | Click for larger image Click to view slides for entire chapter |
 | Click for larger image Click to view slides for entire chapter |
At the end of 2006 the percentage of waiting females, 62%, was the highest observed in 10 years, up from 55% at the end of 2004 though up only slightly from 2005 [Table 12.1a]. The percentage of deceased donor lung transplants performed in females reached a 10-year low in 2006 at 44%, down from 50% in 2004, but little changed from 2005 [Table 12.4a]. Since the death rate for females on the waiting list has been consistently lower than that for males over the past 10 years, this distributional change may be a consequence of sicker patients being selected for transplantation as assessed by LAS factors and not a sex-related effect.
First-year Post Transplant death rates were generally lower for females than males throughout the decade. Total deaths on the waiting list and following transplantation decreased for females from 2004 (610) to 2005 (600). Total deaths for males also decreased by 3% for males from 2004 (562) to 2005 (547) [Table 12.3 and SRTR analysis].
[TOC]There has been minimal variation in ethnic makeup of the active waiting list over the past 10 years. [Table 12.1a]. Hispanic patients had much higher waiting list death rates than whites, African Americans, or Asians in 2006 [Table 12.3]. This higher death rate cannot be explained by a difference in proportion between candidates and recipients, as both groups were 5% Hispanic in 2006 [Tables 12.1a and 12.4a]. The median time-to-transplant was longer for Hispanic patients (192 days) than for whites (128 days) and African Americans (132 days), but not Asians (262 days) [Table 12.2]. Death rates in the first year after lung transplant were within random variation for Hispanic, white and African American patients, although the death rate was lowest for African Americans . The 2005 death rate for Asian patients was particularly poor (517 deaths per 1,000 patient years), but this rate is based on very small numbers [Table 12.7a]. White patients continue to make up the majority of patients waiting (86%) and being transplanted (85%) [Tables 12.1a and 12.4a].
Immunosuppression Therapy After Lung Transplantation
[TOC]Induction therapy was used for 57% of all lung transplants performed in 2006, up from only 22% of lung transplants in 1997 [Table 12.6a]. The induction therapies used most commonly in 2006 were basiliximab (Simulect) (24%) and daclizumab (Zenapax) (16%). In 1997, antithymocyte globulin induction therapy (was used for 20% of transplants and was by far the most common therapy. In 2006, baseline therapy prior to discharge included corticosteroids (97%), tacrolimus (Prograf®, Astellas Pharma US, Deerfield, IL) (83%), and an antimetabolite — either azathioprine (Imuran®, GlaxoWellcome, New Zealand) (39%) or mycophenolate mofetil (Cellcept®, Roche, Nutley, NJ) (52%)) [Table 12.6e]. Calcineurin inhibitor use has changed dramatically — from the predominant use of cyclosporine (Neoral® or Sandimmune, Novartis, East Hanover, NJ) (75%) in 1997 to tacrolimus (83%) in 2006 [Table 12.6e]. In 2005, maintenance immunosuppression administered for the first year following transplantation was essentially the same as immunosuppression before discharge, except that the use of tacrolimus increased from 76% to 86% and the use of sirolimus increased from 1% to 8% of lung transplants [Tables 12.6e and 12.6g]. The immunosuppressive agent most commonly used to treat acute rejection within the first year after transplant was corticosteroids, used in 95% of acute rejection cases [Table 12.6i].
Center and Donor Lung Transplant Outcomes
[TOC]Centers with a volume greater than 21 transplants per year had higher five-year unadjusted graft and patient survival rates (53% and 56%, respectively) than did lower-volume centers (39%-48% and 45%-51%, respectively) [Tables 12.10a and 12.14a]. Recipients of lungs from donors aged 18-34 had the best unadjusted five-year patient survival rates (56%), aside from recipients from donors <1 (71%, based on small numbers). Recipients of lungs from donors aged 65 and above had the lowest patient survival (47%).
[TOC]After falling steadily from 164 candidates at the end of 1997 to only 45 at the end of 2005, the number of patients on the active waiting list for a heart-lung transplant increased slightly in 2006, to 53 patients [Table 13.1a]. These numbers are very small compared to the 1,327 [Table 11.1a] active heart waiting list patients and 1,032 [Table 12.1a] active lung waiting list patients. The death rate on the waiting list in 2006 (143 per 1,000 patient years at risk) was significantly lower than it was in 1997 (284) [Table 13.3].
Only 31 heart-lung transplants were performed in 2006, down from a high of 62 in 1997 [Table 13.4]. Nearly half the heart-lung recipients were aged 35-49, and the most common diagnoses were PPH and congenital heart disease. There were 54 transplant centers that performed heart-lung transplants at some point between 1997 and 2006, but only 15 performed a combined transplant in 2006 [Table 13.17]. The death rate in the first year following heart-lung transplantation dropped to a 10-year low in 2006 [Table 13.7]. Adjusted patient survival rates at three months, one year, three years, and five years were, respectively, 83%, 76%, 56%, and 49%. The five-year survival rate of 49% is similar to that of lung transplant recipients, but the short-term and mid-term survival is much lower than for either heart or lung transplantation [Tables 13.12, 11.12, and 12.12].
[TOC]1. Garrity ER, Moore J, Mulligan MS, Shearon TH, Zucker MJ, Murray S. Heart and Lung Transplantation in the United States, 1996-2005. Am J Transplant 7(5):1390-1403, 2007.
2. Egan TM, Murray S, Bustami RT, Shearon TH, McCullough KP, Edwards LB, Coke MA, Garrity ER, Sweet SC, Heiney DA, and Grover FL. Development of the New Lung Allocation System in the United States. Am J Transplant 6:1212-1227, 2006.
3. Punch JD, Hayes DH, LaPorte FB, McBride V, Seely MS. Organ Donation and Utilization in the United States, 1996-2005. Am J Transplant 7(5):1327-1338, 2007.